Periodontics is the branch of dentistry that deals with the diagnosis and recovery of structures supporting the teeth (periodontal). Parodont consists of the gums (gingiva), bone and fibers that bind a tooth to the bone (periodontal attachment).
Gingivitis is an inflammatory change, which is limited to the gingiva (gums). The inflammatory reaction develops in response to bacterial plaque placed along the neck of the tooth. During the inflammatory reaction it comes to cell damage of the epithelial attachment, and due to it the connection with the surface of the teeth gradually weakens. Then the first signs of gingivitis – bleeding are visible. It happens when tooth brushing and flossing, and in the case of severe gingivitis even during chewing.
However, bleeding encourages patients to “save” the area around the neck of the tooth daily oral hygiene, i.e. to lower brush or avoid the use of floss. Due to weaker hygiene it comes to further accumulation of plaque which will cause even more inflammation, and thus even more bleeding. This closes the vicious circle in which gingivitis and bleeding encourage all poor oral hygiene, and poor hygiene favors strengthening inflammation and bleeding. Other changes that are visible in the case of gingivitis can be redness and swelling of the gums. Gingiva loses its rough texture "orange peel" and becomes shiny, red and tense. These changes become visible only in a more pronounced form of gingivitis.
In milder forms of gingivitis there are no other visible changes, except the bleeding. Therefore, the only sign that accompanies all forms of gingivitis is bleeding (from least to most difficult), making it the most important criterion in diagnosing gingivitis. By treating gingivitis and maintaining good oral hygiene, the damaged epithelial attachment is fully recovered. All the damages occurring during gingivitis are reversible, and it is also the main difference to periodontitis, in which even after treatment permanent damage to periodontal persist.
The main cause of gingivitis is plaque bacteria that cause inflammation. However, there are forms of gingivitis "that are not caused by plaque" and that sometimes can occur during pregnancy and puberty.
Hormonal changes alter the reactivity of the defense system and cause a tendency to develop gingivitis already in the smallest amounts of plaque. Therefore, in this period of life for some people there is an increased risk of gingivitis, even with very good oral hygiene. During the treatment it is necessary to combine professional plaque removal with intense oral hygiene at home. These measures need to be implemented until the hormone levels do not return to "normal". Upon completion of puberty or pregnancy, an increased tendency for gingivitis stops.
A special type of gingivitis can occur when using certain drugs whose side effects increase the gingiva. These are most commonly phenytoin (a medicine for epilepsy), nifedipine (medicine against high blood pressure and heart rhythm disturbances) and cyclosporine (a drug to prevent rejection of transplanted organs), and other medications. These drugs do not cause gingivitis directly, but due to the increase and proliferation of gingival they lead to difficulties in removing plaque in the dental neck. Due to increased accumulation of plaque, gingivitis develops and further increases swelling and gingival overgrowth.
This form of gingivitis is usually treated by replacing the drug which has caused it by another drug that has a similar effect, but does not affect the proliferation of the gingiva.
Periodontitis is an inflammatory change that affects the deeper layers of periodontal - alveolar bone, cementum and periodontal ligament. Periodontitis always develops from gingivitis. When the bacteria are found below the epithelial attachment, they created so-called subgingival plaque that is extremely resistant to daily oral care. Bacteria protected within the subgingival plaque freely grow and reproduce, and the plaque partially mineralizes and it comes to subgingival calculus. It cannot be removed by any "home" measure of oral hygiene, but only by a professional cleaning. Subgingival plaque and calculus allow the development of a large number of bacteria in the area below the gingival margin, in the so-called gingival pocket.
Due to the action of bacterial enzymes and toxins, but also his own defense response, it gradually comes to damage to the deeper periodontal tissues. The alveolar bone is resorbed ("disappeared") and the alveoli is becoming shallower and periodontal fibers are broken down and separated from its attachment to the root and the alveolar bone. Thus, the tooth loses the system that fixes it in his bed, and when the damage becomes extensive, the support of the teeth becomes weak and he becomes loosened.
The division of periodontitis by the speed of progression:
1) Aggressive periodontitis usually occurs in puberty or adolescence. It appears suddenly, and has a significant hereditary component. It progresses and leads to loss of supporting structures of young permanent teeth. A quick and decisive treatment is necessary together with intensive oral hygiene at home to stop the inflammation and prevent its recurrence.
2) Chronic periodontitis occurs later in life, usually after 40-years of age. It progresses more slowly (over several years), and in the course thereof there are quiet periods and acute attacks, sometimes with pus, swelling, pain and bad breath. And this form of periodontitis causes irreversible damages of teeth, and if not treated in a timely manner, it can lead to their loss.
The division of periodontitis according to the extent:
1) Localized - affects up to 30% of all tooth surfaces
2) Generalized –affects more than 30% of the surfaces
The division according to the severity of periodontitis:
1) initial
2) medium
3) advanced
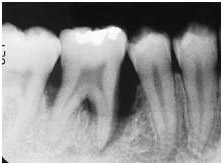
As the most prominent change is observed bone loss around the teeth and part of the "bare" root which is located above the level of the bone. The bone is resorbed due to the inflammatory process, and the tooth has lost part of periodontal fibers that have been connected to the area of roots.
Periodontal abscess is extremely painful and urgent phenomenon that occurs as a result of untreated periodontitis. This is a collection of pus that forms in the periodontal space, and manifests itself as a painful swelling in the roots of the tooth. Gus occurs during severe inflammatory reactions, consisting of decomposed residues of bacteria and damaged tissue. The thick liquid is yellowish in color and odor. When periodontitis progresses in depth or hole pockets shut, pus cannot drain so it comes to a periodontal abscess. Therapy: urgently allow leakage of pus that can be done through the opening of pocket or surgically. After draining the pus and the cessation of symptoms it is necessary to spend treatment of advanced periodontal disease that caused the formation of abscesses. There is a chronic form of abscesses, which manifests itself in the formation of fistulas- "pimples" through which the accumulated pus is draining. Because the pus is drained and does not accumulate, no abscess can be developed, as well as no swelling and pain.
Inflammatory periodontal disease, gingivitis and periodontitis, are the result of interactions between bacteria and plaque defense forces of the organism. Much of the damage to periodontal causes a defensive reaction of the organism, and not only the bacteria. Thus, the tendency to develop periodontal disease is genetically determined and is thus to be assessed on the basis of family history. Patients with extremely severe forms of periodontal disease often have parents who also had periodontitis.
In the past few years tests have been developed that can be used to some extent to determine the reactivity of the defense system of the body, and therefore prone to developing periodontitis. They determine the activity of certain genes and biochemical compounds essential for the regulation of inflammation. However, due to the large number and the complex interaction of all components of the inflammatory response, these tests are not very reliable and rarely applied in practice. Therefore, to predict the tendency of suffering of periodontal disease the family history is still most important. Patients with a family history who have a tendency to the formation of periodontal disease, should pay special attention to a thorough and regular oral hygiene and regular checkups at the dentist, in order to timely recognize this disease and take all therapeutic options.